Understanding SIBO and restoring balance to the gut
Do you often feel inexplicably bloated, your stomach constantly gurgles and rumbles, and you have no idea why? SIBO could be the culprit. The abbreviation stands for Small Intestinal Bacterial Overgrowth and describes an imbalance of bacteria in the small intestine . These aren't "bad" bacteria, but rather beneficial gut bacteria that have simply proliferated in the wrong place – and are causing quite a bit of chaos.
What is SIBO and why is your stomach rebelling?
Imagine your digestive tract as a well-organized city. The large intestine is the bustling marketplace, where trillions of beneficial bacteria live, breaking down fiber and producing essential nutrients. The small intestine, on the other hand, is more of a quiet residential area. This is where the majority of nutrient absorption takes place, which is why it should naturally be quite low in bacteria.
In SIBO, the following happens: The noisy partygoers from the marketplace (large intestine) move to the quiet residential area (small intestine). Once there, they devour food that should actually be digested much later – primarily carbohydrates and sugars. They begin to ferment these nutrients far too early, producing gases such as hydrogen and methane.
The core problem with SIBO: This massive gas production takes place in the small intestine, an organ that is simply not designed for such quantities of gas. The result is painful pressure, leading to the typical SIBO symptoms.
From bloating to irritable bowel syndrome
This bacterial imbalance triggers a whole cascade of symptoms that can severely restrict your quality of life. The consequences of gas formation are often extremely unpleasant and go far beyond a simple feeling of fullness.
- Severe bloating: Your stomach feels like a fully inflated balloon, especially shortly after eating.
- Abdominal pain and cramps: The gases stretch the sensitive small intestine wall and cause pain.
- Changes in bowel movements: Depending on which gases dominate, diarrhea (often with hydrogen dominance) or constipation (typical with methane dominance) may occur.
- Frequent burping: The pressure in your abdomen is finding its way upwards. If you want to learn more about the causes of stomach pressure, read our article on frequent burping and stomach pressure .
SIBO and its close connection to irritable bowel syndrome
Do these symptoms sound familiar? Many of them sound suspiciously like irritable bowel syndrome (IBS), which is why it's often misdiagnosed. The overlap is so significant that experts now believe a large proportion of IBS diagnoses are actually due to undiagnosed SIBO.
It is estimated that small intestinal bacterial overgrowth (SIBO) is the underlying cause in up to 60 percent of the over eleven million people in Germany with irritable bowel syndrome (IBS). This finding is a real game-changer and opens up entirely new treatment approaches for those affected.
Understanding that your bloated stomach isn't just a "quirk of nature" but has a concrete, biological cause is the first and most important step. It's not about you doing anything wrong. It's about an imbalance in your gut that can be addressed.
How to correctly interpret the most common SIBO symptoms
Do you often feel like an overinflated balloon, especially after eating? Do you struggle with sudden diarrhea or debilitating constipation without being able to find a clear trigger? These aren't just your body's whims. They're signals, and it's worth paying close attention. The symptoms of SIBO can be extremely varied and often resemble those of other digestive problems.

The main culprits behind all this chaos? Gases. Imagine the bacteria in your small intestine throwing a wild party with the carbohydrates from your food. The result of this party is gases like hydrogen (H₂) and methane (CH₄) , which create enormous pressure in the sensitive small intestine.
Depending on which bacteria and gases predominate, the symptoms can vary greatly. And this understanding is key to correctly interpreting your body's signals.
The direct line to the gut: hydrogen versus methane
The type of gas produced directly influences how your digestion functions. There are two main types, each with its own characteristic symptoms.
- Hydrogen-dominant SIBO (SIBO-D): When primarily hydrogen-producing bacteria are at work, they draw water into the intestine. This greatly accelerates intestinal transit and typically leads to frequent, sudden, or chronic diarrhea .
- Methane-dominant SIBO (IMO): Methane-producing microorganisms (so-called archaea) cause the exact opposite effect. Methane gas slows down intestinal motility, leading to persistent constipation, severe bloating, and painful gas . This is often referred to today as intestinal methanogen overgrowth (IMO).
The symptoms of SIBO are therefore not a coincidence. They are the direct consequence of the metabolic activity of the bacteria in the small intestine and provide initial important clues about the nature of the imbalance.
Of course, it's also possible that both types of gas are produced in a mixture. The result is often a frustrating alternation between diarrhea and constipation. These symptoms frequently resemble those of food intolerances. If you're unsure which foods trigger your symptoms, a comprehensive intolerance test can finally help you gain clarity.
When SIBO extends beyond the intestines
The effects of small intestinal bacterial overgrowth (SIBO) don't just stay in the gut. The bacteria compete with your body for vital nutrients and can damage the intestinal lining. As a result, nutrients like vitamin B12, iron, and fat-soluble vitamins are no longer properly absorbed.
This nutrient deficiency and chronic inflammation can trigger a whole range of symptoms throughout the body – symptoms that you might not immediately associate with the gut.
These so-called systemic symptoms are often diffuse and difficult to attribute to a specific cause:
- Unexplained tiredness and exhaustion: A deficiency in B vitamins or iron simply robs you of your energy.
- Concentration problems (“brain fog”): Certain metabolic products of bacteria can cross the blood-brain barrier and cloud your thinking.
- Skin problems: Rashes, rosacea or acne can be a direct reflection of an imbalance in the gut.
- Joint pain: Chronic inflammatory processes in the intestine can spread to the entire body.
- Mood swings: The gut-brain axis is a sensitive connection; intestinal problems can exacerbate anxiety or depressive moods.
To give you a better overview, we have summarized the most common symptoms in a table. It distinguishes between local symptoms that occur directly in the abdominal cavity and systemic symptoms that can affect the entire body.
SIBO symptoms at a glance
This table summarizes the most common local (gastrointestinal) and systemic (whole-body) symptoms of SIBO.
| Symptom category | Common complaints | Possible explanation |
|---|---|---|
| Local (gastrointestinal tract) | Bloating, feeling of fullness, belching | Gas production (hydrogen, methane) through bacterial fermentation in the small intestine. |
| Diarrhea (often with SIBO-D) | Hydrogen gas draws water into the intestines and accelerates intestinal transit. | |
| Constipation (common in IMO) | Methane gas slows down intestinal movement and leads to hard stools. | |
| Abdominal pain, cramps | Stretching of the intestinal wall by gases and fluid. | |
| Heartburn, reflux | Increased pressure in the abdominal cavity forces stomach acid upwards. | |
| Systemic (whole body) | Chronic fatigue, exhaustion | Nutrient deficiency (e.g., vitamin B12, iron) due to malabsorption. |
| "Brain fog", concentration problems | Toxic bacterial byproducts enter the bloodstream. | |
| Skin problems (acne, rosacea) | Chronic inflammation and a permeable intestine ("leaky gut"). | |
| Joint pain | Systemic inflammatory reactions originating in the gut. | |
| Mood swings, anxiety | Disrupted communication along the gut-brain axis. | |
| Unintentional weight loss | Inadequate intake of calories and nutrients. |
This variety of signs shows how crucial a healthy gut is for your overall well-being. If you recognize yourself in this mosaic of symptoms, you're not alone. It's a clear indication that it's time to give your digestion the attention it deserves.
Uncovering the hidden causes and risk factors
A SIBO diagnosis is an important step, but it's rarely the root cause of the problem. Think of it this way: the bacterial overgrowth is usually just the loudest symptom of a much deeper underlying issue. To effectively manage SIBO, you have to play detective and find out why the bacteria were even able to proliferate in the small intestine in the first place.
Imagine your small intestine has a built-in cleaning function – a kind of "cleaning wave" that sweeps through regularly. This ensures that food residues and bacteria are reliably pushed on to the large intestine, preventing any build-up in the small intestine. If this self-cleaning mechanism fails, perfect chaos ensues, allowing bacteria to multiply explosively.
When the intestines' engine goes out of rhythm
The most important mechanism for this cleansing process is the so-called Migrating Motor Complex (MMC) . This is a powerful, wave-like muscle contraction that travels through the small intestine whenever you're not eating – that is, between meals. The MMC is essentially your intestine's natural cleaning crew.
The MMC is activated approximately every 90 to 120 minutes in an empty stomach. Any small snack in between immediately interrupts this cycle and prevents the small intestine from being effectively cleared.
If this rhythm is disrupted, bacteria and food scraps simply remain. There, they have all the time in the world to multiply and produce gases. A whole range of factors can paralyze this crucial mechanism, thus paving the way for SIBO.
Structural problems and medications as disruptive factors
Sometimes, very real mechanical or medication-induced changes are what tip the balance. These are among the most common and clearly identifiable triggers of SIBO.
- Adhesions after surgery: Scar tissue in the abdominal cavity, for example after an appendectomy or a cesarean section, can actually constrict the small intestine or restrict its freedom of movement.
- Impaired stomach acid production: Stomach acid isn't just for digestion. It's one of your most important barriers against germs and kills a large proportion of the bacteria you ingest with food.
- Chronic stress: Prolonged stress puts your body into "fight or flight" mode. In this state, digestion is deemed unimportant and simply shut down – which also paralyzes the MMC and reduces the production of stomach acid.
Long-term use of proton pump inhibitors (PPIs) is a significant risk factor. Studies show that this dramatically increases the risk of small intestinal bacterial overgrowth (SIBO), especially in older patients. Approximately 30 percent of patients who take PPIs for extended periods develop SIBO. Without the protective acid barrier, bacteria have virtually free rein. You can read more about the research findings in this area here.
Underlying diseases as silent drivers
SIBO is also often an unwelcome companion of other chronic diseases. In these cases, treating the underlying disease is the real key to keeping SIBO under control in the long term.
- Celiac disease or gluten intolerance: The chronic inflammation in celiac disease can damage the nerves in the intestine that are responsible for regulating the MMC (myeloproliferative cell). You can learn more about this connection in our article on celiac disease and gluten intolerance .
- Crohn's disease: This chronic inflammatory bowel disease can also severely impair the structure and motility of the intestine.
- Hypothyroidism: Thyroid hormones regulate the pace of life throughout the body. If they are lacking, metabolism slows down, and with it, the entire digestive process.
- Diabetes: Persistently elevated blood sugar levels can damage nerves over time (diabetic neuropathy). This can also affect the nerves responsible for digestion.
Finding the root cause is the most important part of the entire SIBO journey. Only by identifying and addressing the true trigger can you prevent the symptoms from recurring. It's about restoring your gut's ability to heal itself.
SIBO diagnosis: How to find out if you are affected
You have a feeling your symptoms might indicate SIBO, but how do you get certainty? The path to the correct diagnosis can seem a bit confusing at first, but don't worry. We'll go through it together step by step. This way, you'll know exactly what to expect and can go into your appointment with your doctor or therapist well-prepared.
It all starts with a thorough medical history . Here, an expert carefully examines your symptoms, medical history, and lifestyle. This is crucial to rule out other possible causes for your symptoms and to confirm a suspected case of small intestinal bacterial overgrowth (SIBO).
This infographic shows you the typical process – from the first signs to the tangible result.
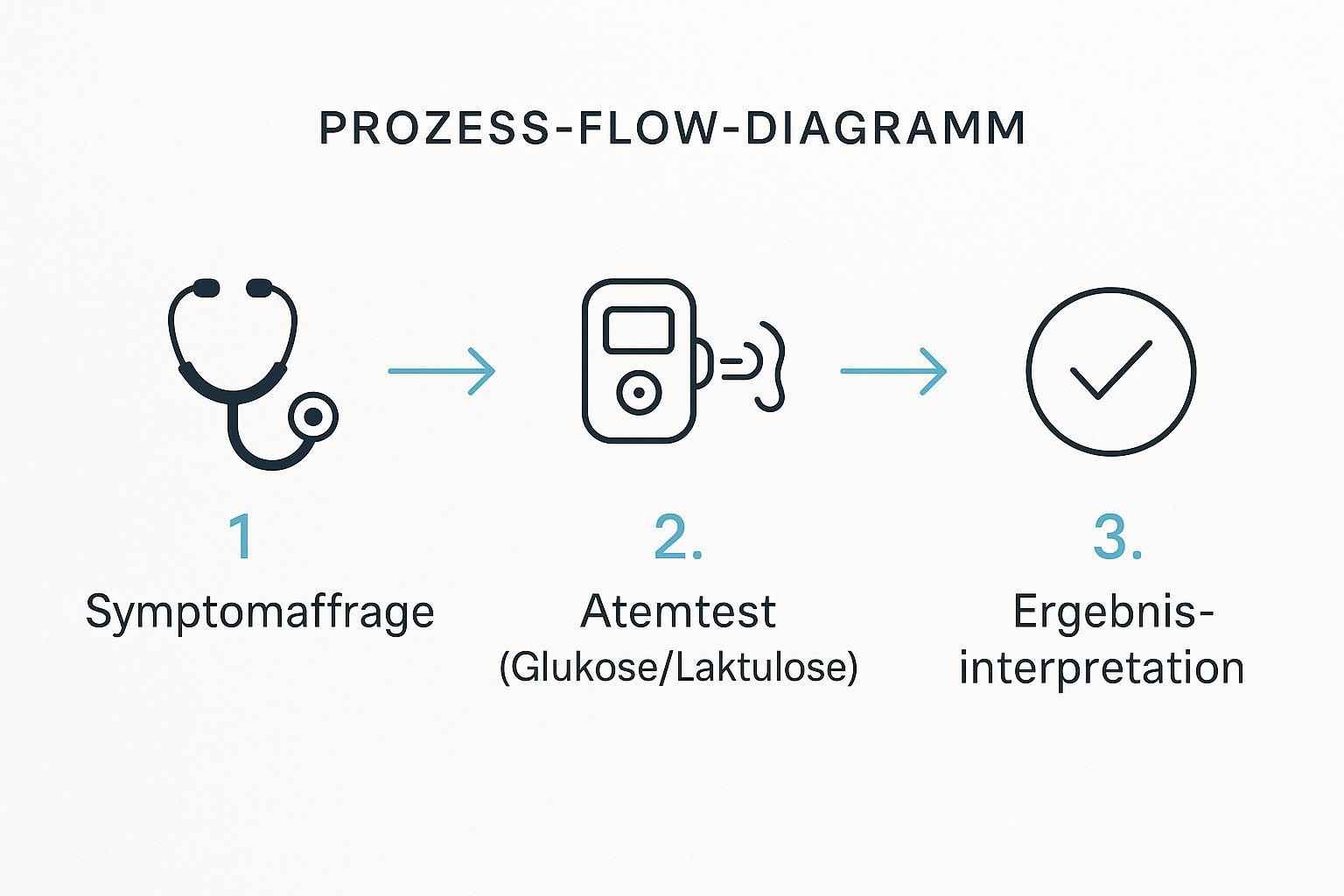
As you can see, the process is structured very logically and ultimately leads to a crucial test that should finally bring clarity.
The breath gas test: How to detect bacteria
If SIBO is suspected, the so-called breath gas test is the method of choice. It is considered the non-invasive and reliable gold standard for detecting bacterial overgrowth in the small intestine. The idea behind it is quite clever: you simply measure the gases produced by the bacteria directly in your breath.
And this is how the test works:
- Baseline measurement: First, you blow into a device while fasting to determine the normal gas content of your breath.
- Drinking a sugar solution: You will then be given a special sugar solution to drink. This is usually either lactulose or glucose.
- Blow regularly: Over the next two to three hours, blow into the measuring device again at fixed intervals (e.g. every 20 minutes).
The sugar solution is essentially "food" for the bacteria. If there are too many of them in the small intestine, they immediately devour it and begin to ferment the sugar. This process produces gases such as hydrogen (H₂) and methane (CH₄) . These gases enter your bloodstream and travel to your lungs, where you exhale them. A significant increase in these gases in your breath is then the decisive evidence.
What the test result really means
You'll have a positive result if the concentration of hydrogen or methane rises sharply within the first 90 to 120 minutes after drinking the solution. This early rise is the key criterion. It shows that fermentation is already taking place in the small intestine – and not later in the large intestine, where it actually belongs.
The magnitude and precise timing of the gas increase provide valuable clues. A rapid and significant rise indicates a problem in the upper part of the small intestine. If the levels rise later, the colonization is likely located further down the intestine.
To ensure the test is truly meaningful, you need to prepare well. That's absolutely crucial. Generally, this means:
- Special diet: One to two days before the test, there is a very restricted diet with as few fermentable carbohydrates as possible.
- Sobriety: You must be completely sober on the day of the test.
- Medication break: Certain medications, especially antibiotics or laxatives, often need to be discontinued weeks in advance.
Your doctor or the lab will give you very specific instructions. It's essential that you follow them! This is the only way to ensure that the result truly reflects your current bowel condition and that the diagnosis is based on a solid foundation.
Treating SIBO holistically: Your roadmap to gut health
A SIBO diagnosis is not an end point, but the starting point for taking control of your gut health again. It's not simply about eliminating a few bacteria. Rather, we want to create a healthy balance that lasts in the long term. A truly successful treatment rests on four pillars that mesh together like gears in a machine.
The first step is usually to end the excessive bacterial growth in the small intestine. There are various ways to do this, which must be tailored to your individual needs. Only then can your gut finally calm down and begin to regenerate.
Pillar 1: Contain bacterial overgrowth
To reduce the number of unwanted guests in the small intestine, we need to decrease their numbers. Both conventional medical and herbal methods have proven effective for this.
- Antibiotics: The most well-known approach is treatment with the antibiotic rifaximin . Its major advantage: It acts almost exclusively in the gut and barely enters the bloodstream. This largely protects the important microbiome in the large intestine.
- Plant-based alternatives: Herbs such as oregano oil , berberine , or neem are true powerhouses of nature. They have strong antimicrobial properties and have proven to be a very effective alternative in practice. They are often combined to target the broadest possible spectrum of bacteria.
Interestingly, there are currently no official S3 guidelines for the treatment of SIBO in Germany. Therapy therefore relies heavily on the experience of specialists and is individually tailored. Rifaximin is officially approved in Germany only for traveler's diarrhea, which complicates matters.
Pillar 2: Proper nutrition as a powerful ally
Alongside reducing the bacteria, your diet plays a key role. Imagine simply cutting off the bacteria's supply by depriving them of their favorite food source – without neglecting important nutrients yourself.
The low-FODMAP diet is one of the best-known strategies here. FODMAPs are certain carbohydrates that are like a feast for SIBO bacteria. By reducing them, you essentially "starve" the bacteria. The result is often rapid relief from bloating and pain.
Very important: A low-FODMAP diet is a short-term therapeutic measure, not a long-term diet! In the long run, it can restrict the diversity of your beneficial gut bacteria in the large intestine. Therefore, you should definitely seek guidance from a healthcare professional.
Pillar 3: Tackling the root cause to prevent relapses
This is perhaps the most important step of all. Because SIBO is almost always just a symptom of a deeper problem. Once we have the overgrowth under control, we have to ensure that it doesn't flare up again immediately.
This is where the Migrating Motor Complex (MMC) – your gut's "cleaning wave" – comes into play again. To reactivate it and boost natural bowel movements, prokinetics are used. These can be herbal remedies like ginger or certain medications. They help your gut to cleanse itself again.
Pillar 4: Building a sustainable gut microbiome
Now that we've cleaned things up, your gut is ready to rebuild. The next step is to promote good bacteria and heal the intestinal lining so it becomes strong and resilient again.
This is where probiotics come into play. During the acute reduction phase, they can sometimes do more harm than good. But afterwards, they are indispensable for specifically repopulating the gut flora and restoring balance. The key is to use the right bacterial strains at the right time.
Gradually, prebiotic fiber can be reintroduced to specifically feed the beneficial bacteria in your large intestine. A detailed analysis of your microbiome can show you exactly where to start. Learn how a comprehensive microbiome test can help you take your gut health to the next level.
Questions and answers about SIBO
If you're researching SIBO, you'll likely have a lot of questions swirling around in your head. That's perfectly normal, because the road back to a healthy gut is rarely a straight line. To help you gain some clarity, we've compiled the most frequently asked questions.
We want to give you understandable and practical answers. This will help you better understand the connections and take the next steps on your path in an informed and confident manner.
Can SIBO disappear on its own?
This is a question many sufferers ask themselves with hope. The honest answer, however, is: in the vast majority of cases, unfortunately, no. The reason for this is actually quite logical: SIBO is rarely the actual problem, but usually only a symptom of a deeper underlying disorder.
Imagine it like a burst water pipe in the basement. SIBO is the water flooding the basement. You can keep bailing out the water, but as long as the leak—the root cause—isn't repaired, the basement will keep flooding. It's the same with SIBO. A short-term diet might alleviate the symptoms because you're giving the bacteria less food. But the underlying cause, the bacterial imbalance, remains.
Without targeted therapy that both reduces the bacteria and addresses the root cause of the problem – such as impaired bowel motility (MMC) – the symptoms are highly likely to return. Long-term success requires a holistic approach .
What role do probiotics play in SIBO?
Probiotics are an important but also tricky topic when it comes to SIBO. Timing is crucial. Most experts advise against taking probiotics during the acute phase, when the goal is to reduce the bacteria in the small intestine. The reasoning behind this is that you don't want to introduce even more bacteria into an already overcrowded system.
Once the bacterial load has been successfully reduced, the situation looks very different. Then, high-quality probiotics are a crucial component for specifically rebuilding the gut flora and strengthening the healthy balance in the large intestine.
They help stabilize the intestinal barrier and prevent relapse. So it's not a question of "yes" or "no" to probiotics, but rather about the right timing and selecting the appropriate bacterial strains for your situation.
How long does SIBO treatment take?
Patience is likely your most important companion during SIBO therapy. The duration is extremely individual and depends heavily on the severity of the colonization, the underlying cause, and your overall health. It's not a sprint, but rather a marathon with several stages.
- Phase 1: Reduction The pure fight against bacteria with antibiotics or herbal remedies usually takes between two and six weeks .
- Phase 2: Addressing the Root Cause & Prevention This part is often the longest. Getting the intestinal motility (MMC) back on track and treating the underlying cause can take several months.
- Phase 3: Rebuilding Rebuilding a healthy gut flora sustainably and allowing the intestinal mucosa to heal is also a process that can take months.
Overall, you should be prepared for the entire journey from diagnosis to a stable, symptom-free condition to take anywhere from six months to over a year . But every single step is worth it for your quality of life.
The path to a better gut feeling begins with understanding your body. At mybody-x , we support you in gaining sound insights into your gut health. With our scientifically based analyses, you'll discover what your microbiome is lacking and receive the tools to specifically improve your well-being. Discover the possibilities now at https://mybody-x.com .


Share:
Leaky Gut Syndrome: What's really behind it
Leaky Gut Nutritional Therapy: Your Path to a Healthy Gut