Rebuilding gut flora after antibiotics: Here's how you can really succeed
You've just finished a course of antibiotics, but you still feel a bit sluggish and your stomach is acting up? You're not alone. Antibiotics are often lifesavers, but they have one crucial drawback: they not only wipe out the harmful bacteria in your gut, but also countless beneficial bacteria. Therefore, rebuilding your gut flora is the most important step to getting back on your feet quickly and understanding your body's signals.
Why your gut needs support after antibiotics
Imagine your gut microbiome as a vibrant, blooming garden. Trillions of tiny microorganisms, primarily countless strains of bacteria, live there in a finely balanced equilibrium. They aid digestion, produce vital vitamins, and provide round-the-clock training for approximately 70% of your immune system .
Antibiotic therapy sweeps through this garden like a chemical weed killer. Sure, the disease-causing bacteria – the "weeds" – are effectively eliminated. But unfortunately, countless beneficial "flowers and herbs" are simply uprooted along with them. What's left is a rather bare bed with significantly less biodiversity.
Collateral damage in the microbiome
Some groups of bacteria, which play a key role in your health, are particularly sensitive to this:
- Bifidobacteria: These hardworking little bacteria are incredibly important for the production of short-chain fatty acids. These, in turn, nourish your intestinal lining and keep inflammation in check.
- Lactobacilli (lactic acid bacteria): They create a slightly acidic environment in the gut. This makes it very difficult for pathogens to colonize and thrive there. They also help you digest lactose.
Broad-spectrum antibiotics, in particular, can drastically reduce these and other beneficial strains. A scientific analysis has shown that drugs like doxycycline or azithromycin can virtually wipe out entire populations of important gut bacteria. Others are "only" inhibited in their growth. If you want to delve deeper into the subject, you can read the results here.
The noticeable effects on your body
The absence of protective bacteria is like an open invitation for unwanted guests. Yeast fungi such as Candida or the bacterium Clostridioides difficile suddenly have free rein. They can proliferate in the empty spaces and cause new problems.
The effects of a weakened gut flora aren't limited to digestion. An imbalance can affect your entire body – from your skin and energy levels to your mood.
Your body sends pretty clear signals when its internal ecosystem is out of balance. These can be obvious things like bloating or diarrhea, but also a higher susceptibility to the next infection or that feeling of constant exhaustion.
This table shows you at a glance how antibiotic therapy can affect your gut and your overall health in the short and long term.
Direct effects of antibiotics on your body
| Affected area | Typical effect | Why this is important to you |
|---|---|---|
| Gut flora (microbiome) | Reduction of bacterial diversity and number of beneficial strains. | A less diverse microbiome is more susceptible to pathogens and is less able to utilize nutrients. |
| digestion | Diarrhea, bloating, abdominal cramps (antibiotic-associated diarrhea). | Digestive function is impaired, leading to direct discomfort and poorer nutrient absorption. |
| immune system | Weakening of the immune system, since approximately 70% of immune cells are located in the gut. | You become more susceptible to new infections – a vicious cycle can begin. |
| Nutrient supply | Reduced production of important vitamins (e.g., vitamin K, B vitamins). | A deficiency can lead to fatigue, poor concentration, and other vague symptoms. |
| Long-term risks | Increased risk of chronic inflammation, allergies, or irritable bowel syndrome. | A disrupted intestinal barrier ("leaky gut") can promote long-term health problems. |
To fully understand the importance of a healthy gut flora, it can also be interesting to look at how the topic of gut health is treated in dogs , as the basic principles are often surprisingly similar.
This knowledge is the foundation for everything that follows. You will soon learn how to specifically provide your gut with the right building blocks and create an environment in which your beneficial bacteria can re-establish themselves and multiply. It's about bringing your inner garden back to life.
The truth about probiotics after antibiotics
After a course of antibiotics, many people almost reflexively reach for a pack of probiotics. It sounds logical, doesn't it? The "good" bacteria have been destroyed, so we simply replenish them. But unfortunately, it's not that simple. The blanket recommendation "Just take probiotics" is scientifically outdated and, in the worst-case scenario, can even backfire.
Imagine your gut after antibiotic treatment like a freshly plowed field. The colorful diversity of plants that has grown over years is gone. If you now sow masses of seeds from just one type of flower, it will quickly fill the open spaces, but at the same time, it will crowd out the many native species that would naturally grow back.
The well-intentioned attempt to quickly replenish your levels can therefore block the natural and far more important regeneration of your individual microbiome. Instead of restoring the original diversity, you create a new, but less diverse, monoculture.
The delay effect of probiotics
This paradoxical effect is not just a theoretical concept. A groundbreaking study presented at the Internal Medicine Update in Hamburg investigated precisely this phenomenon. Researchers compared three groups after a course of antibiotics: one received probiotics, one a fecal transplant, and the third nothing at all. The result was astonishing: the group without any special treatment had restored its original microbiome after about 60 days. The probiotic group, on the other hand, had not regained its former balance even after 180 days – half a year.
Routine use of the medication significantly slowed down natural recovery. You can learn more about these fascinating research findings and understand why experts advise caution today.
This finding does not mean that probiotics are inherently bad. It simply depends on the right timing and the right application.
When probiotics can still provide targeted help
There are specific situations in which taking selected probiotic strains is absolutely beneficial. However, the focus here is not on general recovery, but on preventing or treating a specific problem.
- For the prevention of antibiotic-associated diarrhea (AAD): This is the best-studied use. Certain strains have been shown to reduce the risk of diarrhea during antibiotic therapy.
- To suppress specific pathogens: They can help keep harmful germs like Clostridioides difficile in check, which tend to spread after a course of antibiotics and cause severe diarrhea.
Two strains with proven efficacy
| bacterial strain | Main effect when taking antibiotics | Important NOTE |
|---|---|---|
| Lactobacillus rhamnosus GG | It has been proven to reduce the risk of diarrhea by stabilizing the intestinal barrier and displacing harmful germs. | One of the best-researched probiotic strains worldwide, with a solid data foundation. |
| Saccharomyces boulardii | A medicinal yeast that is particularly effective against the toxins of pathogens and protects the intestinal mucosa. | Because it is a yeast, it is not directly attacked by the antibiotic and can be taken at the same time. |
The crucial point is this: instead of blindly reaching for a broad-spectrum probiotic to rebuild gut flora after antibiotics , it's much wiser to focus on the actual goal. Far more important than adding new bacteria is nourishing the remaining beneficial bacteria and helping them grow.
The foundation for this is primarily laid by bifidobacteria and lactobacilli, which are often particularly vulnerable to antibiotic treatment. You can read more about the key role of bifidobacteria and lactobacilli in our follow-up article.
Ultimately, the best strategy is to give your body the right tools so it can restore its unique flora on its own. We'll look at exactly how that works in the next step: your diet.
Your diet as the foundation for rebuilding
Now that it's clear why reaching for probiotics without thinking isn't always the smartest idea, we come to the absolute heart of your recovery. The best and most sustainable method for rebuilding your gut flora after antibiotics starts right on your plate. Imagine the beneficial gut bacteria that survived the course of antibiotics as a small group of starving survivors. They now urgently need the right food to multiply and quickly repopulate the gaps that have been created.
The image of an overgrown garden fits perfectly here: Instead of simply throwing a few new seedlings (probiotics) into the ground and hoping they'll grow, you first take care of the soil. You give it the best nutrient mix (prebiotics) so that the robust, native plants that are still there can sprout vigorously. In this way, a strong, resilient ecosystem develops all by itself.
Prebiotics: The superfood for your gut
The key to this nutrient boost lies in prebiotic foods . These are special, indigestible fibers that, while offering no direct nutritional value to you, are a veritable feast for your beneficial gut bacteria, such as bifidobacteria and lactobacilli. They act almost like a highly effective fertilizer for your microbiome.
These valuable helpers are found in many everyday foods:
- Leeks and garlic are absolute powerhouses of prebiotics. Even a small onion in a sauce or some leeks in soup makes a noticeable difference.
- Root vegetables: Jerusalem artichokes, chicory, parsnips and black salsify are particularly rich in inulin , one of the most effective prebiotics.
- Other vegetables: Asparagus and artichokes also provide valuable food for your little helpers.
- Legumes: Lentils, chickpeas and beans are not only protein bombs, but also excellent sources of fiber.
- Whole grain products: Oat flakes, barley and rye bread contain beta-glucans, which specifically stimulate the growth of beneficial bacteria.
- Cold starch: A brilliant trick! Cooked and then cooled potatoes, pasta, or rice develop resistant starch. This acts like a prebiotic and is a delicacy for your gut flora. So a cold potato salad is not only delicious but also very gut-friendly.
Fermented foods as natural helpers
Besides "food," you can also give your gut direct support in the form of fermented foods. These naturally contain live bacterial cultures that can gently support your gut flora – without blocking natural regeneration, as high-dose supplements sometimes do.
Unlike isolated bacterial strains in capsules, fermented foods provide a natural diversity of microorganisms within a matrix of nutrients. This often makes them more easily tolerated by your gut and more sustainably effective.
Try to regularly include these foods in your diet:
- Natural yogurt & kefir: Look for products without added sugar and with the note "contains live cultures".
- Sauerkraut: Be sure to choose fresh, unpasteurized sauerkraut from the refrigerated section. Heating it kills the valuable lactic acid bacteria.
- Kimchi: The Korean fermented cabbage is a true bacteria bomb and also brings a pleasant spiciness.
- Kombucha: This fermented tea drink is a great alternative to sugary sodas.
The following table gives you a quick overview of which foods you should pay particular attention to right now.
The best foods for gut health
Here is a clear list of gut-friendly foods that specifically support your recovery. We have divided them into "food" (prebiotics) for your existing bacteria and "helpers" (fermented foods) with new microorganisms.
| Food category | Concrete examples | This is how they work in your gut |
|---|---|---|
| Prebiotics (food) | Onions, garlic, leeks, asparagus, artichokes, Jerusalem artichokes, chicory, rolled oats, legumes, cooled potatoes | They provide indigestible fiber that serves as food for your good gut bacteria, promoting their growth and reproduction. |
| Fermented food (helper) | Natural yogurt, kefir, unpasteurized sauerkraut, kimchi, kombucha, cloudy apple cider vinegar | They provide a natural diversity of live microorganisms that gently enrich your microbiome and support recolonization. |
By incorporating a good mix of both categories into your diet, you create the ideal conditions for a quick and sustainable regeneration of your gut.
What you should avoid now
Just as important as what you eat is what you consciously avoid. After a course of antibiotics, your gut is particularly sensitive. Certain foods can disrupt regeneration or even feed the wrong, unwanted microorganisms.
The top 3 disruptive factors:
- Sugar and white flour: They act like fertilizer for harmful yeasts (e.g., Candida) and bacteria, which are just waiting to thrive in the empty spaces. Swap sweets for a handful of berries and white bread for a slice of whole-wheat bread.
- Highly processed foods: They are often full of artificial additives, emulsifiers, and sugar. All of this can irritate the intestinal lining and promote inflammation. Cook fresh meals as often as possible. A simple lentil stew is quick to make and a real treat for your gut.
- Excessive alcohol: Alcohol can directly attack the intestinal lining and negatively affect the delicate balance of the gut flora. Give your body a break and, during the recovery phase, opt for water and unsweetened herbal teas instead.
A conscious, gut-friendly diet is the most important building block for restoring balance to your microbiome. If you'd like to delve deeper into this topic, you'll find further valuable tips and recipe ideas in our comprehensive guide to building gut flora nutrition . This isn't about a short-term diet, but about giving your body the best possible foundation for lasting healing.
How your lifestyle affects gut healing
Proper nutrition is essential for rebuilding your gut flora after antibiotics . But it's only half the battle. Your body is a complex system where everything is interconnected. Factors like chronic stress, poor sleep, and insufficient exercise can significantly sabotage your gut's regeneration process—no matter how gut-friendly your diet is.
Imagine trying to create a beautiful garden, but constantly battered by a storm. That's exactly what happens in your gut when your lifestyle isn't in harmony with its healing processes. A holistic approach is therefore key to success.
Stress as an invisible adversary
Chronic stress is one of the biggest enemies of a healthy gut. When you're constantly under pressure, your body releases more of the stress hormone cortisol . And this hormone seriously disrupts your digestive system.
It can reduce the protective mucus layer of your intestinal wall and loosen the connections between intestinal cells. This condition, often referred to as "leaky gut," makes your gut more permeable to substances that don't belong there. At the same time, stress alters the composition of your microbiome and promotes the growth of less beneficial bacteria.
The good news is: You don't have to completely turn your life upside down. Even small, conscious breaks in everyday life can make a huge difference.
- The 4-7-8 breathing technique: Inhale through your nose for 4 seconds, hold your breath for 7 seconds, and exhale slowly through your mouth for 8 seconds. Repeat this 3-4 times whenever you feel overwhelmed.
- Short nature breaks: A 15-minute walk in the park or forest during the lunch break has been proven to lower cortisol levels.
- Digital detox: Consciously put your smartphone away for an hour in the evening. This helps your nervous system to finally calm down.
Sleep – your body's repair shop
While you sleep, your body is anything but inactive. The gut, in particular, uses this time for intensive repair and regeneration processes. The cells of the intestinal lining renew themselves at a rapid pace, and the immune system recalibrates.
Lack of sleep brutally disrupts these important processes. Studies show that even a few nights of poor sleep can negatively affect the diversity of gut bacteria. The goal should be 7–8 hours of high-quality sleep per night.
Your gut has its own internal clock. A regular sleep rhythm – meaning going to bed and getting up at roughly the same time, even on weekends – helps to synchronize this clock and optimize the healing processes.
The following infographic summarizes the process of gut restoration in three simple steps: Avoid what harms, feed what helps, and help with the right cultures.
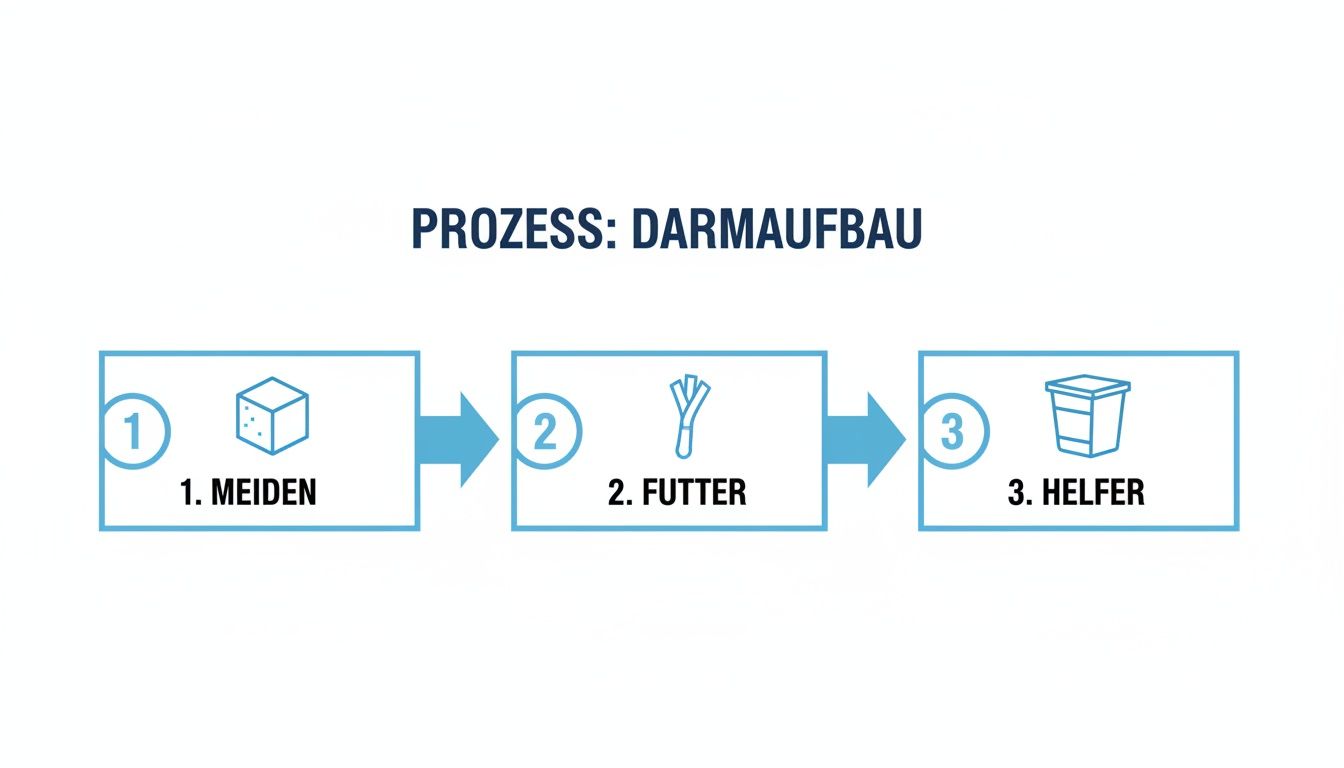
The visualization makes it clear: Rebuilding is an active process that requires conscious decisions regarding diet and lifestyle.
Movement – gentle stimulation
Moderate exercise is another important component. It not only stimulates bowel activity and can thus help with constipation, but it also promotes blood flow to the intestinal wall. This improves nutrient supply and supports healing.
The key here is moderation. Extreme endurance sports can put additional stress on the intestines. Gentle, regular activities are ideal during the recovery phase.
- Brisk walking: 30 minutes a day is perfect to get your digestion going.
- Yoga or Pilates: Gentle twists massage the internal organs and can stimulate intestinal peristalsis.
- Cycling: A joint-friendly way to activate the circulatory system without overloading the body.
Your lifestyle creates the environment in which your nutritional efforts can truly bear fruit. By reducing stress, ensuring good sleep, and engaging in moderate exercise, you create a safe and nourishing environment for your microbiome, allowing it to optimally recover and flourish.
When a test after a course of antibiotics really makes sense
You're doing your best – diligently eating your oatmeal, avoiding sugar, and going for regular walks. But how do you know if your efforts are really paying off? Is your body getting everything it needs for a quick recovery? Instead of guessing, you can do some targeted research and give your body exactly what it might be lacking.
Imagine it like this: A gut weakened by antibiotics is like a leaky sieve. The intestinal lining, normally an impenetrable barrier, becomes temporarily more permeable. This has two crucial consequences: Nutrients are absorbed less efficiently, and your body suddenly becomes more sensitive to certain foods.
Signs that your body needs more
If you're still struggling with persistent symptoms weeks after finishing a course of antibiotics, these are clear signals from your body. These signs indicate that simply changing your diet might not be enough:
- Persistent digestive problems: bloating, irregular bowel movements or stomach rumbling that just won't go away.
- Unexplained fatigue: You sleep enough, but still constantly feel tired and lacking in energy.
- Skin problems: Pimples, eczema or a sallow complexion can be a reflection of your gut health.
- Cravings for sweets: A strong desire for sugar can indicate an imbalance in the intestines, where yeast fungi have proliferated.
- Increased susceptibility to infection: If you go from one cold to the next, your gut-based immune system could be weakened.
These symptoms aren't just annoying. They can point to deeper deficiencies or triggers that are subtly sabotaging your training plan. This is precisely where mybody-x's self-tests can provide valuable insights and help you shift from a general approach to a personalized strategy.
Targeted insights instead of blind guesswork
The good news is that the gut flora usually recovers. A Swedish study showed that the bacterial community typically regenerates almost completely within six months after antibiotic therapy. However, even after this time, some protective strains were permanently missing. Especially in Germany, where around 17 million courses of antibiotics are prescribed annually, this demonstrates how important targeted support is.
A mybody-x test helps you understand exactly what is happening in your body during this sensitive phase.
The mybody-x nutrient test
A damaged gut can no longer efficiently absorb important vitamins and minerals such as zinc, magnesium , or B vitamins . These nutrients are essential for repairing the intestinal lining and for the proper functioning of your immune system.
A nutrient test can reveal whether you have a deficiency. Instead of buying expensive supplements on suspicion, you can specifically replenish the nutrients your body really needs.
The mybody-x food intolerance test
Sometimes, certain foods can silently cause persistent irritation in the gut and hinder healing. After a course of antibiotics, your body may react to foods that you previously tolerated without any problems.
An intolerance test (IgG4 test) identifies precisely these potential culprits. By deliberately avoiding these foods for a while, you give your intestinal lining the necessary rest to fully recover. This is often the crucial factor in finally getting rid of persistent bloating and discomfort.
When is the right time to get tested?
The ideal time for a test is not immediately after finishing the last course of antibiotics. Give your body three to four weeks to begin the initial stages of recovery through basic dietary and lifestyle changes.
If you still feel like you're stuck in a rut afterward, or if the symptoms mentioned above persist, it's time to dig deeper. The results will provide you with a data-driven foundation to optimize your post-antibiotic gut flora restoration plan. They replace guesswork with facts and put you back in control.
Although mybody-x doesn't offer direct stool analysis, you can learn more about the different analysis options available and how they complement each other in our article about microbiome testing . Ultimately, the goal is to specifically address the consequences of an imbalanced gut flora and provide your body with the best possible, personalized support.
Frequently asked questions about gut restoration after antibiotics
You've now thoroughly researched how to specifically support your gut health. Even so, you might still have a few questions. That's perfectly understandable! Here I've compiled the most frequent and important questions we receive – short, concise, and straight to the point.
How long does it really take for my gut flora to recover?
That's the question that everyone is probably dying to know. The regeneration time is very individual and depends on many factors. Studies suggest a period of about six months until the diversity of your microbiome has largely recovered.
However, your eating habits, the type and duration of antibiotic therapy, and your general lifestyle play a crucial role here. With targeted measures, such as a high-fiber, plant-based diet and conscious stress reduction, you can actively support and often accelerate this process. Patience is key – your gut ecosystem is complex and simply needs time to heal.
Should I start building up my strength while still taking antibiotics?
That's a good question! While you're taking antibiotics, it's best to focus on easily digestible and nutrient-rich foods. Think steamed vegetables, light soups, and easily digestible carbohydrates to ease the strain on your body.
Targeted rebuilding with a wealth of prebiotic foods is most effective immediately after the end of antibiotic therapy. The reason is simple: the nutrients and fiber you consume are no longer affected by the antibiotic. This gives the remaining beneficial bacteria the best possible head start to multiply again.
Imagine it like sowing seeds in a garden. You also wait until the heavy rain (the antibiotic) has stopped before sowing the seeds (prebiotics). This way, they won't be washed away and will find the best conditions to grow.
What symptoms indicate a disturbed gut flora?
Your body's signals can vary greatly. There are some classic signs, but also more subtle indications that can point to an imbalance in the gut.
Typical symptoms include:
- Digestive problems: Persistent bloating, irregular bowel movements (diarrhea or constipation), abdominal rumbling or a constant feeling of fullness.
- Energy & immune system: Unexplained, persistent fatigue and an increased susceptibility to infections.
- Skin & Mood: Skin problems such as acne or eczema, as well as sudden mood swings or concentration problems.
If these symptoms persist for weeks after finishing your course of antibiotics, that's a clear sign. Your gut needs extra support, and it's worth taking a closer look.
Can I directly analyze my gut flora with a test from mybody-x?
This question is particularly important for understanding how our tests work. mybody-x does not offer a direct microbiome analysis that lists the exact composition of your bacterial strains. Instead, we focus on the consequences of an imbalanced gut flora – because these are what you experience in everyday life.
A damaged intestine can cause two main problems:
- Impaired nutrient absorption: The intestinal lining is irritated and can no longer optimally utilize vitamins and minerals. Our nutrient test detects precisely these kinds of deficiencies.
- Increased sensitivity: A weakened intestinal barrier can cause you to react adversely to certain foods. Our intolerance test helps you identify these potential culprits.
These tests allow you to specifically address the consequences of dysbiosis. You discover what your body is lacking or what is irritating it, thus indirectly but very effectively supporting the healing of your gut. It's a solution-oriented approach that helps you personalize your treatment and regain balance more quickly.
Do you want to gain clarity on how your course of antibiotics has affected your nutrient intake or potential food reactions? At mybody-x, you'll find scientifically sound at-home self-tests that provide precise insights. Discover the right tests for you now and take control of your health: Learn more at mybody-x.com



Share:
The role of nutritional tests – for individual health
Get your microbiome tested easily at home